Connective Tissue Diseases
The connective tissue diseases consist of rheumatoid arthritis, lupus erythematosis, dermatomyositis, scleroderma, periarteritis nodosum and serum sickness. All of these can have significant dermatologic manifestation. Of these six, the three so-called collagen diseases; lupus, dermatomyositis and scleroderma will be discussed here. They are considered autoimmune diseases (the body reacts against itself).
Lupus

There are several forms of lupus erythematosis which can affect the skin with or without internal involvement.
Discoid lupus erythematosis (DLE) presents with red, scaly plaques which develop atrophy (loss of skin substance) with scarring, loss of hair and pigment changes. The lesions normally occur on the sun-exposed areas of the body particularly the face, upper torso and scalp. Therapy is usually quite effective, but scarring is often permanent if treatment is delayed.
Subacute cutaneous lupus erythematosis (SCLE) normally presents with more dramatic and extensive skin lesions, involving sun-exposed areas and with multiple circular or geometrically varied lesions on the back or upper torso.
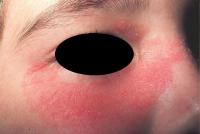
Acute LE usually presents with a seriously sick patient, often with a butterfly rash over the face and on sun-exposed areas along with fever, weakness, arthritis, and a host of other systemic findings. The quicker this illness is diagnosed and treated, the better the patient chances are for full recovery
Click here for more
pictures of lupus
Dermatomyositis
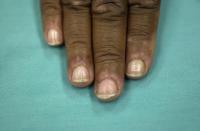

Dermatomyositis is a serious disease involving the skin and muscles. It can occur in children, adults and in association with malignancies. The onset is usually abrupt, often following sun exposure with progressive muscle weakness and the development of a skin rash. Most diagnostic findings of the skin changes occur on the face and hands. Swelling around the eyes, often with dermatitis with a peculiar heliotrope (purplish) coloration. The changes on the hands are reddish plaques or flat-topped violaceous papule-like lesions. This occurs over the backs of the fingers, known as Gotton’s papules, sparing of the skin between the knuckles. Telangiectasia, fine blood vessels, involving the cuticles of the nails is often found.
Click here for more
pictures of
dermatomyositis
Scleroderma
Scleroderma (hard skin) occurs in several forms. Localized scleroderma is commonly called morphea, which can develop at any age and presents itself with solitary or multiple reddish smooth patches on the body which are firm to touch. As the lesions progress, they expand with a violaceous border that gradually hardens in the center. The lesions are usually asymptomatic.
Linear scleroderma is commonly referred to as coup de sabre (blow of the sword). A significant loss of tissue can be seen and can be quite disfiguring.
CREST syndrome is a limited variation of scleroderma. CREST is an acronym for the common features of the disease, Calcinosis, Raynauds, Esophageal dysmobility, Sclerodactyly (thickening of skin over fingers), Telangiectasia (fine blood vessels on the face, mouth and hands).
Systemic scleroderma often has similar skin findings, along with significant internal problems especially involving the lungs, kidneys and gastrointestinal tract. Therapy often requires a multidisciplinary approach.
Click here for pictures
of scleroderma

