Herpes Simplex
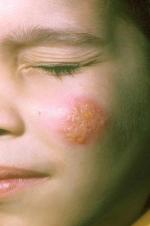
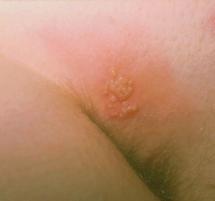
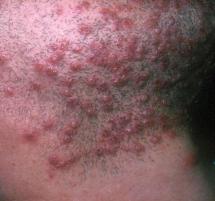
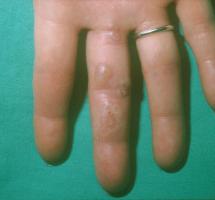
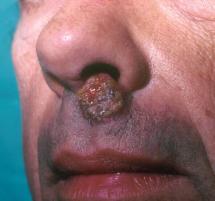
One of the more common problems encountered in dermatology practice is herpes simplex (also known as cold sores). Cold sores are caused by the herpes virus, either Type 1 or Type 2. The virus enters the skin through some opening in the epidermis, often secondary to trauma. It then replicates in the skin and within a few days produces itching, tenderness and mild discomfort in the involved area. This is rapidly followed by swelling and redness. Within 24 to 48 hours, multiple grouped blisters appear. The blisters soon become cloudy, then develop a purulent (pimple-like) character with subsequent erosion and crust formation. An enlargement and tenderness of a local or regional lymph node may develop simultaneously.
Treating Herpes Simplex
There are a variety of therapies available for herpes simplex. The frustrating thing about herpes simplex is that while the therapy is very effective at clearing the skin lesions, however, none of these medications prevent recurrence. Suppressive therapies can be used to prevent recurrences.