Leg Ulcers
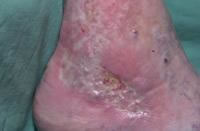

Leg ulcers are a significant problem leading to major inconvenience, discomfort and inability to work or function. Most leg ulcers occur about the ankles and are secondary to varicose veins. This propensity runs in the family and is associated with being overweight in most cases. Leg ulcers often develop after the age of forty in patients who spend a lot of their time on their feet. Phlebitis (blood clots) in patients with leg ulcers is common. These ulcers are called stasis dermatitis secondary to chronic edema (fluid in the legs) and venous insufficiency. Therapy is very effective for these ulcers. The sooner they are treated, the easier it is for the patient to recover.
The second most common cause of leg ulcers is leukocytoclastic vasculitis. This produces deep, punched out, very painful ulcers with surrounding white scar tissue (atrophe blanche) which is pathognomonic of this condition. These ulcers are tough to heal and are often recurrent.
Arterial ulcers are the third and most difficult ulcers to manage. They result from inflammatory vasculitis of many varied etiologies. Embolization (blocks the flow of blood) can be caused by a blood clot, cholesterol, tumor or arteriosclerosis (thickening and hardening of the arterial walls). An obstructive block (total occlusion) can lead to gangrene (death of tissue). Without sufficient blood supply, tissue dies, and the body is unable to heal these ulcers. Peripheral vascular surgeons are usually required to deal with these problems.
Click here for
more pictures of
leg ulcers

